Concussion: Eye Movements Help in Assessment of Head Injury
Contents |
Concussion: Eye Movements Help in Assessment of Head Injury
Introduction
Head injuries can often cause the trauma to the brain known as concussion; concussion occurs when the head receives a serious blow from a fall, an accident or collision and it happens because the brain floats in fluid within the skull. When the head suffers trauma, the brain is sent crashing into the opposite side of the skull from the blow, causing injury.
It is difficult to definitively diagnose concussion, especially right after the injury, because it doesn’t always show up in traditional testing methods such as CT or MRI scans, according to neuroscientist Uzma Samadani, MD, of the departments of neuroscience, physiology and neurosurgery at New York University’s Langone Medical Center in New York City. She pointed out that it is difficult to tell how badly the brain may be injured after such an event, or even if it has been injured at all. Even if the physician knows there is an injury, it is hard to tell whether the injury is getting better or worse over time.
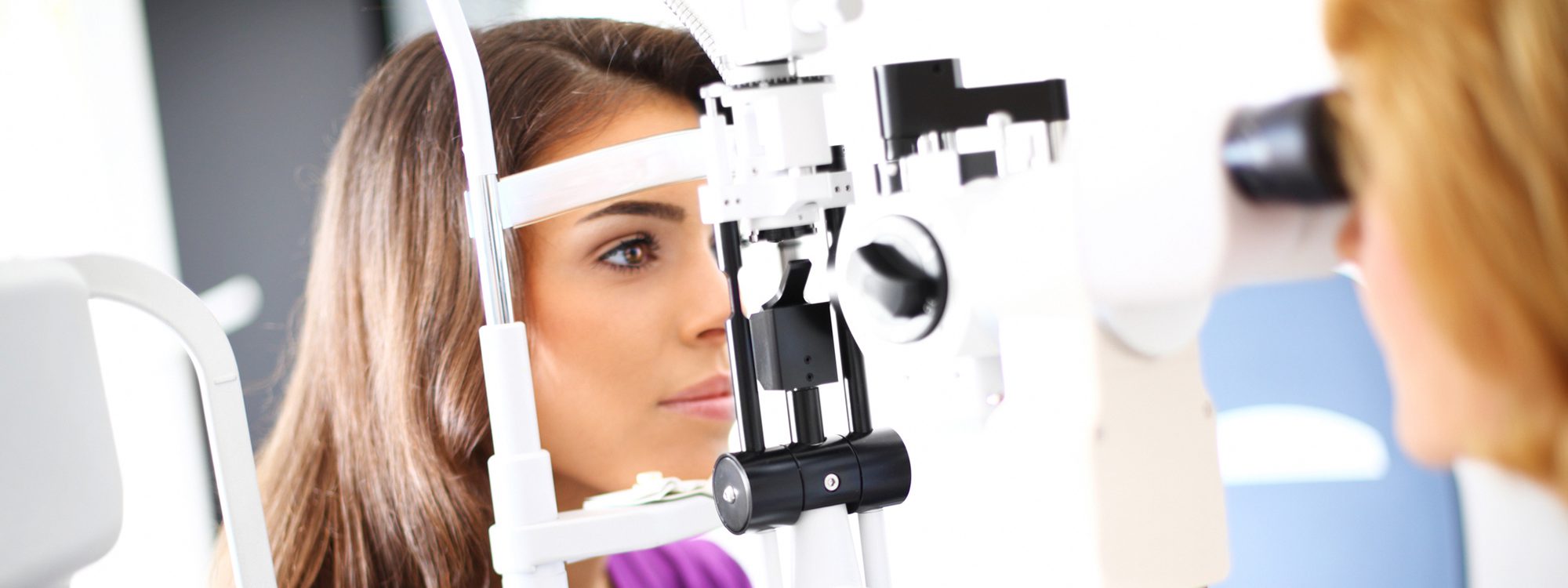
Right : By tracking the location of the pupillary reflexes, (the white dots that appear from the reflection of a light off the front of the eye, seen here as two bright white dots) eye movement tracking can help in the diagnosis and evaluate severity of brain concussion injuries.
Every 8 seconds in North America, someone gets a serious blow to the head, severe enough to cause concussion. Because the best technologies – the scans noted above – can’t always detect concussion, a better, more reliable way to assess possible damage is badly needed. Assessing the level of damage is important because a second injury while the brain is healing itself from a previous one can cause much more damage, a situation that might arise at a sports event, for example, when there is a tendency for both coaches and players to downplay the seriousness of their injuries and a desire to continue to participate in the game.
Such a method may become available soon, using computer software that tracks the movement of the eyes while the injured person watches television.
Testing
Dr. Samadani’s team started with the idea that patients with more severe injuries would not be able to watch television, as someone without concussion would. They came up with software that would track eye movements by tracing where the pupils of the eyes tracked a moving object without error and easily, or if one eye lagged even a fraction of a second behind the other. In tests, healthy people could do so, but those with brain injuries could not.
Additionally, in many patients, the discontinuation of the eye movements in tracking across a screen revealed not only that injury was present, but where in the brain it might have occurred. It is possible that this new testing method may finally be the way to detect concussion but to find out how severe it is.
From this initial trial, the team found a neurodiagnostic company, Oculogica, which loaned its testing platform, called EyeBox, to the Children’s Hospital of Philadelphia (CHOP) concussion center.
The EyeBox does not need calibration that some other systems require, so a child with an injury doesn’t have to sit through that process; it also evaluates whether both eyes are tracking accurately together, where some other systems only look at one eye with the assumption that what one eye does, the other does also. As noted above, however, that is not always the case in brain trauma.
Concussion in children apparently results in the same type of eye movement abnormalities and the severity of the injury as it does in adults.
Christina Master, MD an attending physician at CHOP and a specialist in pediatric sports medicine thinks this idea has merit and significant implications. During the last year, Dr. Master saw about 3000 children for concussion, which is an increase from five years ago. Most of these children had eye movement and tracking problems.
The primary “job” of children is to attend school and to learn. In modern school systems, this is heavily dependent on visual processing of information. If there is a breakdown of visual skills, as in concussion, there will be a breakdown in learning as well.
The technology allows doctors to see subtle differences between normal and abnormal scores to use in evaluating balance and visual issues and would allow schools to compensate for any deficits found.
Future Plans
Currently, there are prototypes of the EyeBox system set up in three locations at New York University, and one is being installed at Fort Campbell, KY, home of the 101st Airborne Division of the US Army, for use in evaluating damage after blast injuries.
If these results are confirmed by other physicians in other studies, this system could be made available in sports arenas, school sports locker rooms and emergency rooms. Results can be made available in as little as three and a half minutes; Dr. Samadani explained. “We could do it in less time, but for now we just like to do multiple repetitions of the testing to confirm these results.” One of the huge advantages of the EyeBox system is that it is not an invasive procedure, unlike testing spinal fluid or blood, and it eliminates the subjective aspect of testing of eye tracking that is possible when different clinicians perform the physical examination.
Plans have been made to submit the system to the US Food and Drug Administration for further testing by other physicians to replicate her findings.
Summing Up
It has been known for some time that the eyes and eye movements are helpful in testing for impaired function of the brain. Field sobriety tests, for example, often include a test for tracking skills to detect eye movement breakdowns when tracking an object from side to side at extreme gaze. Called endpoint nystagmus, the eyes begin to lose the ability to stay on target and become erratic.
Also, one quick test for possible concussion is to look at the relative size of one pupil to the other. Differences don’t always show up there, because concussion occurs in different areas of the brain, but when pupil size differences are present, it is usually a good assumption that some type of injury has occurred.
Being able to quantify and standardize eye movement disorders is a huge step up in the determination of the presence of concussion injury. It will allow for conclusive evidence to both coaches and players, for example, to discover these injuries and to know that the injured player should be taken out of the game to avoid further injury and worse damage.
Better diagnosis of concussion and its severity is a very worthy goal.