Amblyopia and Lazy Eye
Contents |
Amblyopia and Lazy Eye
It is estimated that about three percent of children less than six years of age have some form of amblyopia, which causes decreased vision in the affected eye. Also known as Lazy Eye, amblyopia is considered to be the most common form of vision loss in childhood.
To understand amblyopia and its causes, it is useful to think of vision as something that occurs in the brain, not just in the eye. Light enters the eye through the pupil and is focused onto the retina. The retina is made of millions of nerves which respond to the light by sending messages to the brain along the optic nerve to the visual cortex, where the brain turns them into images.
The visual cortex develops dramatically in infants and young children, and continues to do so throughout the first decade of life. Amblyopia occurs when something interferes with this process and the brain is unable to develop the ability to interpret the signals coming from the affected eye in the usual way.
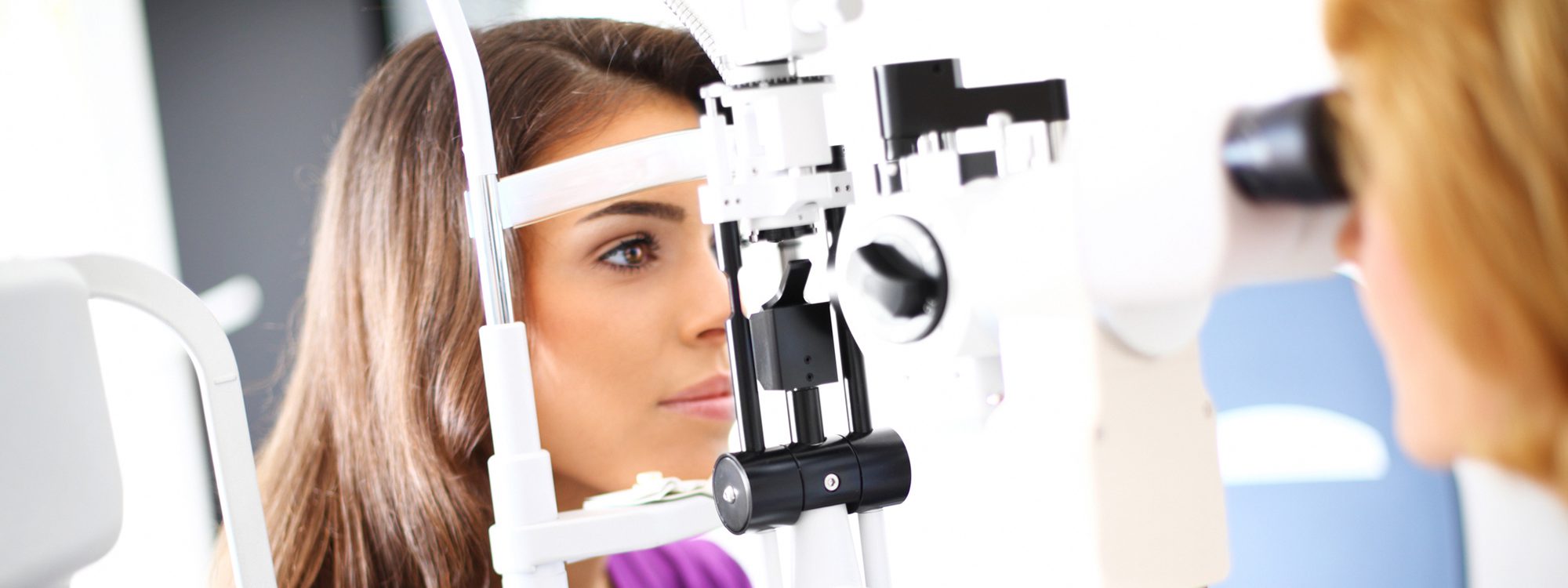
The key to successful treatment of amblyopia is early diagnosis; most visual scientists believe that there is a critical period of vision development, which lasts from infancy until about age eight. If the amblyopia is not diagnosed or treated by the end of this critical time, it is much more difficult to achieve normal visual function. As seen in figure 1, even very young children can have their vision tested; parents should not hesitate to schedule a vision exam before the age of three years.
Children do not know that their vision is abnormal or unusual; they think everyone sees the way they do, and generally do not complain about their vision. However, there are certain symptoms and signs that may be noticed: one eye turning inward or outward; excessive clumsiness and an inability to properly judge distances or a preference for using one eye, usually by covering or closing the other. A family history of amblyopia can also be significant.
Sometimes, one eye turning inward or outward is very noticeable to anyone, but it is also possible to have one eye turned in or out only slightly, without any cosmetic indication at all.
It is important to understand that amblyopia is not just a case of simple blurred vision, but should be thought of as interrupted visual development. Except in very rare cases, a simple lens prescription will not provide normal vision. Full lens correction is usually needed, but unfortunately, lenses by themselves cannot overcome amblyopia.
Two of the most common causes of amblyopia are Refractive and Strabismic.
Refractive Amblyopia
Refractive amblyopia occurs when the refractive error (nearsightedness, farsightedness or astigmatism) in one eye is very different from that of the other, a condition called anisometropia, or when both eyes have significant refractive errors that are not corrected while vision is developing. In anisometropia, mblyopia results when the brain recognizes that the images from one eye are significantly more clear than from the other; it will then adapt itself to the difference in clarity by learning to ignore, or suppress, the central vision from the blurred eye in favor of the one with the best vision.
In rare cases, the refractive error in both eyes may be large enough to cause significant blur at all distances, which can result in failure of the visual system to develop its normal ability to recognize clarity, resulting in functional blindness. It is very important that this condition be diagnosed and treated, the earlier the better.
Treatment consists of correcting the refractive error with spectacles or contact lenses to provide the best possible image so the amblyopia doesn’t develop. The vision specialist will sometimes also advise a course of specific visual exercises to help the brain learn to recognize clear vision more easily.
Strabismic Amblyopia
Strabismus is the name of the condition when eye eyes are not aiming properly as a team; one eye may turn inwards or outwards while the other maintains fixation. With clear vision in both eyes, this misalignment will cause double vision, or diplopia. Because diplopia is very disturbing, the brain adapts by selectively ignoring, or suppressing the central vision of the misaligned eye. The straight eye will usually develop normal vision, while the other may not, resulting in amblyopia.
Treatment of this type of amblyopia includes spectacle correction of any refractive error, vision therapy exercises aimed at overcoming the central suppression and the use of prisms to allow images from each eye to be perceived, thus breaking down the suppression. Patching of the stronger eye to force the weaker one to work and begin to recognize sharp images has also been shown to be helpful. Recent research indicates that patching of the better eye for up to two hours a day is useful in helping to achieve more equal vision, because it forces the weaker eye to work and develop normally. The goal of patch therapy is to break up the adaptation that the brain has made, and make it easier to establish a different, more normal one; therefore, the patch may be used only over the stronger eye, or alternating between the two.
When the misalignment is large, surgical intervention may be needed to adjust the muscles that are responsible for eye movement. Vision therapy and proper lens and/or prism correction will help maintain both functional and cosmetic alignment.
Accommodative esotropia is a special type of strabismus, which involves focusing and aiming together.
Early Diagnosis and Treatment
Amblyopia is considered to be largely preventable, when treated quickly. Early intervention can also restore and reverse vision loss, but when left untreated, an amblyopic eye may become functionally blind and never develop normal vision.
As seen in figure 2, vision examination of toddlers and even infants is possible, with the use of specialized equipment such as the eye chart shown here; sophisticated instruments that can detect the presence of refractive errors such as nearsightedness and astigmatism without the need for the child’s responses to questions at all; and even very simple tools like the always useful paddle-like occluder, which in the hands of your eyecare practitioner can determine if strabismus is present, which eye it affects, and which direction the eye turns.
Because there are often no outward signs or symptoms, it is very important that parents should have their child’s vision examined and evaluated by a vision specialist before the age of three.